Are you expecting a child? Pregnancy is a time of great anticipation and heightened anxiety for expectant mothers and fathers.
This anxiety often focuses on the health of the unborn child – many parents worry about their children being born with genetic disorders.
While the vast majority of babies in the United States are born without any health complications, you may still want to know as much as you can about your baby’s health.
Parents can opt for two types of genetic testing when they’re expecting: invasive testing and non-invasive testing.
While invasive testing may seem like the more traditional and therefore more comprehensive option, it can pose certain risks to a mother’s health.
What Is Invasive Genetic Testing?
As mentioned, invasive genetic testing is the more traditional option for looking for genetic disorders while a baby is in the womb.
The test results are accurate but pose many forms of discomfort to the mother. Doctors can perform this procedure in one of two methods: amniocentesis or chorionic villus sampling.
- Amniocentesis is a procedure in which the doctor will take a needle and place it into the amniotic sac, which is a pouch filled with fluid that protects the baby while in the womb. The doctor will retrieve fluid from the sac and test it for genetic disorders.
- The doctor can perform chorionic villus sampling using one of two methods. The doctor can use a needle and place it through your stomach to retrieve placenta tissue. If you do not want to have a needle in your stomach, the doctor will extract a placenta sample by inserting a tube through your cervix. He or she will then test your placenta for genetic disorders.
What Does Invasive Genetic Testing Look For?
Invasive genetic testing looks for diseases and medical conditions that your baby may develop based on family history.
Certain ethnic groups or people with a family history of certain conditions are at high risk of passing them on to the next generation.
Invasive genetic testing looks for many conditions, such as cystic fibrosis, Down syndrome, and other genetic abnormalities.
The Risks of Invasive Genetic Testing
Invasive genetic testing uses a needle or a tube to collect amniotic or placental samples. As a result, both the baby and the mother may be subjected to pain and discomfort.
Amniocentesis runs the risk of puncturing the amniotic sac, which can lead to an unsafe environment within the womb.
If you opt for this procedure, the puncture will expose your fetus, and it may face developmental consequences.
Chorionic villus sampling can tear or damage your placenta, which your baby needs to survive. This procedure can make the placenta less effective.
In addition, invasive genetic testing can lead to a risk of miscarriage. While the rates of miscarriage are statistically small, any risk of miscarriage is a cause for concern.
Amniocentesis can lead to a miscarriage rate of 1 in 200 to 1 in 400. Chorionic villus sampling can lead to a miscarriage rate of 1 in 100 to 1 in 200.
Alternatives to Invasive Genetic Testing
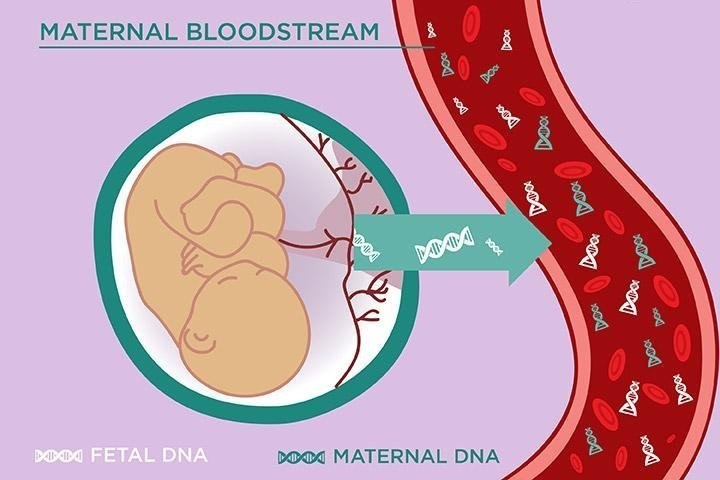
If you do not want to opt for the painful, potentially harmful procedures of invasive genetic testing, non-invasive options are available.

The test is also very effective, and you can receive many types of NIPTs from your doctor, including MaterniT21 PLUS and other options.
If you want to avoid invasive procedures and receive accurate results about your child’s health, opt for non-invasive testing.